|
|
There’s been a bit of activity online regarding LVADs; which is a good thing. I always found them hard to grasp and even harder to find useful information on. So I couldn’t pass this up, when Scott Weingart (EM Crit) posted a summary and podcast on the darned things. He highlights the key things to know about LVADs, along with some links to good reference sites and a really good EMS Field Guide to LVADs, which you must download, print out and stick up on a prominent wall just in case. Check out Scott’s podcast here There’s also a discussion on LVAD development and use available from the Medscape Critical Care Podcast on iTunes (Podcast 17, released on 19 12 2011)
|
They key messages seem to be:
- The patient may not have a palpable pulse (or audible Korotkoff sounds) but still be alert and well perfused, due to the continous flow from the LVAD.
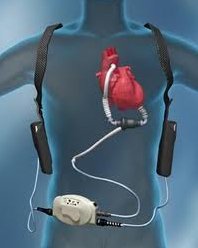
- Follow the cable emerging from the patient’s right upper quadrant (the drive line) and check that all connections to the 2 batteries and the control box are intact. Then check the 2 batteries and the control box.
- Listen over the praecordium for the hum of the pump motor. If none, see above. Gen I VADs had back up hand pumps. Gen II and III devices do not.
- Feel for excessive heat over the position of the motor, suggesting the motor is working really hard -> pump thombosis, suctioning low volume LV chamber, distal obstruction such as aortic dissection.
- If septic and no other source -> Drive line infection until proven otherwise
- RV function supplies LV volume and is critical to an optimally working LVAD
- The patient may have VF, VT or asystole on the ECG monitor yet be conscious, though possibly not for very long. Defibrillation can be safely performed in standard positions. CPR is contentious due to the risk of tube dislodgement, but if the patient is going to die without CPR then it’s hard to criticise.
- Find the contact details of the VAD coordinator or doctor somewhere on the device or in the patient’s support bag and contact them soon.