The latest installment of the NEJM’s critical care series has been published with the results of this months’s poll asking for your opinion on haemodynamic monitoring in severe sepsis.
This new venture has featured an evolving case that has been presented in parts over the past few months, each installment presented with a specific clinical question that you can vote and comment on.
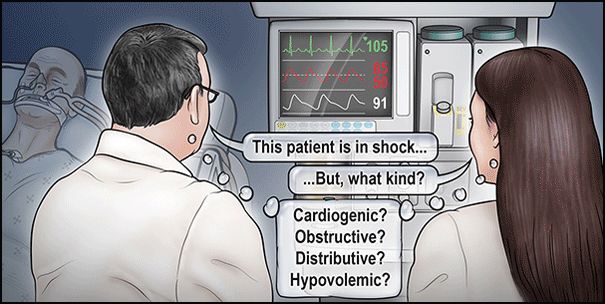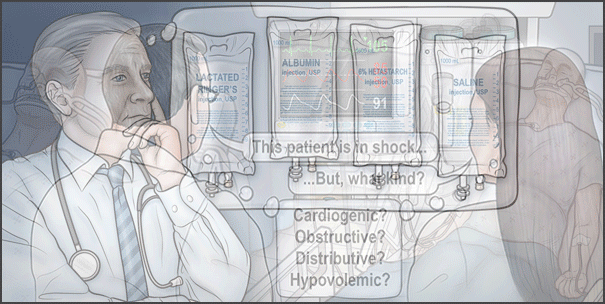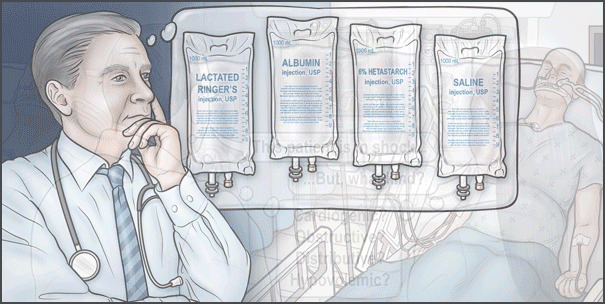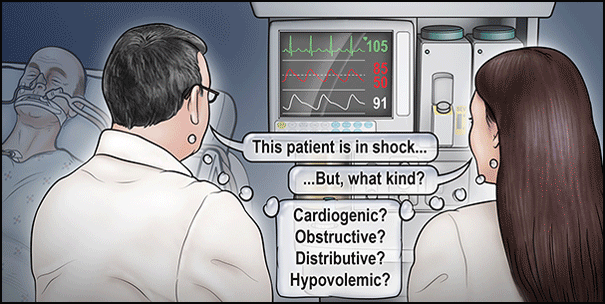
A 77-year-old man is admitted to the intensive care unit (ICU) of a university hospital from the operating room with fecal peritonitis caused by a perforated sigmoid colon. The patient’s medical history includes treated hypertension and hypercholesterolemia, previous heavy alcohol intake, and mild cognitive impairment.
Having been given 4 liters of crystalloid perioperatively, the patient arrives in the ICU hypotensive and tachycardic. He is mechanically ventilated. After a further 1 liter of Hartmann’s solution and 500 ml of 5% human albumin solution he remains hypotensive and tachycardic with a central venous pressure is 9 mm Hg.
At this point the poll asks what monitoring strategies would you use to guide hemodynamic support for this patient?
[/az_box_icon]
As usual, there is an excellent accompanying review article by experts in the field Vincent and De Backer which provides an overview of the pathophysiology and clinical approach to shock as well management and treatment goals. The above monitoring strategies are reviewed as well as the newer means of evaluating microcirculatory flow and tissue oxygenation. The review can be found here.