March 2011
A 24 year old lady, who is normally fit & well, is admitted to ED following a high-speed MVA. She was driving her car at approximately 70kph and was hit from the side by another car.
On arrival in ED, she is complaining of difficulty breathing, with chest and abdominal pain. Her GCS is 15, she has a regular pulse at 122bpm, BP of 105/60mmHg and is well filled peripherally. Her oxygen saturations are 93% on 15L/min of oxygen via reservoir bag. On auscultation, she has reduced air entry to her left base, but no wheeze or crepitations. Her abdomen is globally tender with a seat-belt mark across the skin.
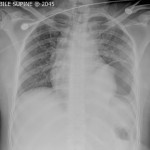
Her admission chest radiograph is shown (click here for full image.)
Questions
- What is the diagnosis from the chest radiograph?
- What is the ultimate management of this condition?
- Given this injury, what other injuries would you be concerned about?
- If she required intubation for hypoxic respiratory failure, what options are there to optimally manage her subsequent ventilation, prior to any ongoing procedures?
Answers
- The chest radiograph demonstrates a gastrothorax. Given the history, this is likely to be due to a traumatic diaphragmatic rupture. Left-sided diaphragmatic rupture occurs twice as common as right-sided rupture, principally due to anatomical differences: the diaphragm is relatively weak on the left and the liver provides more protection on the right. Diaphragmatic rupture occurs in about 1% of blunt thoracic trauma patients, but is reported in up to 8% of those requiring laparotomy following blunt thoracoabdominal injury.
- The ultimate management is surgery, to repair the diaphragmatic injury. Whilst, an isolated diaphragmatic injury could potentially be repaired laparoscopically or thoracoscopically, the usual route where there is a herniated viscus would be via laparotomy. Additionally, a laparotomy would afford the opportunity to optimally manage any other intra-abdominal traumatic organ injuries. Furthermore, from an anaesthetic point of view, a laparoscopically induced pneumoperitoneum may make ventilation challenging given the pre-existing gastrothorax.
- In this case, the combination of the history, diaphragmatic rupture and the seatbelt sign should be taken as an indication of a rapid deceleration and high impact. Consequently, one should be alert to other concomitant injuries, which will tend to occur in >50% of patients with diaphragmatic rupture. Almost any other organ could potentially be injured, particularly within the thorax and abdomen. Certainly splenic injuries are very likely, but also liver lacerations, bowel injuries, rib fractures, haemothorax, pneumothorax, lung contusion, great vessel injuries, cardiac contusion, spinal injuries, closed head injuries, plus long bone and pelvic fractures.
- An orogastric or nasogastric tube to decompress the stomach would facilitate ventilation. A standard single lumen endotracheal tube (ETT) would be optimal. If thoracic surgery is being contemplated, a double lumen ETT would facilitate this. However, usually diaphragmatic rupture is repaired from below, and if thoracic surgery and one lung ventilation are required, a bronchial blocker could potentially be used, or the ETT changed at that stage.
Consequently, a single lumen ETT, using conventional ventilation (6-8mls/kg), would be optimal, with a reasonable PEEP.
References
- UpToDate.com: General approach to blunt abdominal trauma in adults
- UpToDate.com: General approach to blunt thoracic trauma in adults
Feel free to discuss this case in the ICN Forum or post a comment below.
























