The NEJM is running a new series covering some key aspects of critical care and they want your opinion and vote to count in this exciting new venture.
A critical care case is presented with a specific clinical question that you can vote and comment on.
An editorial or review will then follow from a world expert discussing the case and your vote.
The first editorial and introduction to the series is here (for free)
Topics in the series will include:
- Management of severe sepsis
- Choice and use of resuscitation fluids
- Treatment of shock
- Management of delirium
- ICU-acquired weakness
- Recovery from prolonged critical illness
The first case and answer can be found here
Read more for the second case and to see how to cast your vote and comments!
Presentation of Case
A 77-year-old man whose medical history includes treated hypertension and hypercholesterolemia, previous heavy alcohol intake, and mild cognitive impairment is admitted to the intensive care unit (ICU) of a university hospital from the operating room after a Hartmann’s procedure performed for fecal peritonitis caused by a perforated sigmoid colon. He has received a total of 4 liters of crystalloid fluids, which were administered in the operating room. (In the first voting installment, there were 7823 votes regarding treatments that might decrease this patient’s risk of dying from septic shock, with the use of hydrocortisone favored by 78% of respondents, gamma globulin by 11%, and a statin by 9%. In addition, many of the respondents suggested that the patient should receive further fluid resuscitation.)
On arrival in the ICU, the arterial blood pressure is 88/52 mm Hg with marked respiratory variation, the heart rate is 120 beats per minute in sinus rhythm, the central venous pressure is 6 mm Hg, and the temperature is 35.6°C. He is peripherally cool, with prolonged capillary refill. Arterial blood gas results while the patient is receiving mechanical ventilation with a fraction of inspired oxygen of 0.4 are as follows: pH, 7.32; partial pressure of carbon dioxide, 28 mm Hg; partial pressure of oxygen, 85 mm Hg; and lactate, 3.0 mmol per liter. Results of serum biochemical analysis are as follows: sodium, 142 mmol per liter; potassium, 4.4 mmol per liter; chloride, 109 mmol per liter; urea, 22.0 mg per deciliter (7.9 mmol per liter); creatinine, 2.3 mg per deciliter (203 µmol per liter); and albumin, 23 g per liter. The urine output during the last 2 hours in the operating room was 28 ml.
Question
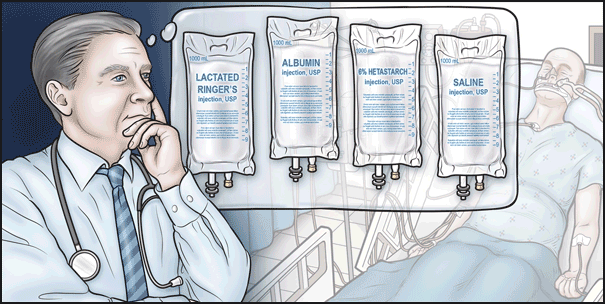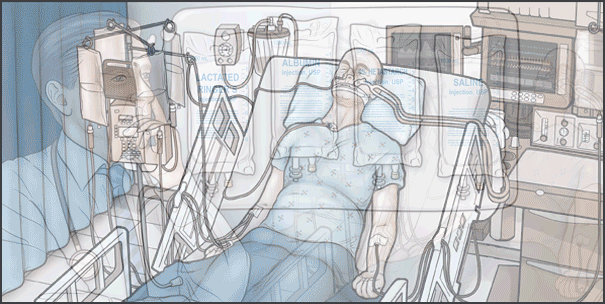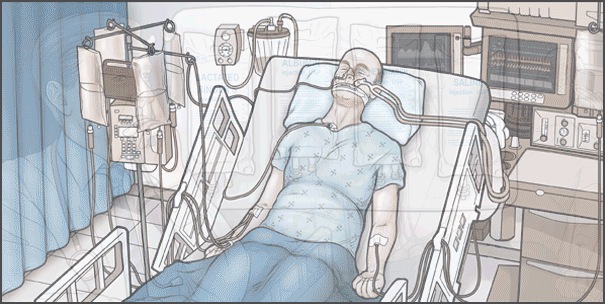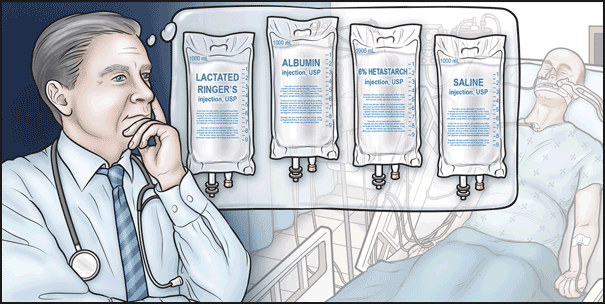
After an assessment showing that the patient has inadequate intravascular volume, what fluid resuscitation would you choose to be administered over the next 30 minutes to 1 hour?
Participate in the poll and submit a comment supporting your choice.
Watch out for the poll results and the review article in a couple of weeks!

























