SCANNING THE VENTRICLES
PRE-READING FOR THE FCUS COURSE
Contents
- Scanning the ventricles: the questions to ask
- Qualitative or quantitative? The Goldilocks Approach.
- Is LV size big / small / grossly normal?
- Is RV size big / small / grossly normal?
- RV: increased size versus increased pressure
- Is LV contraction increased / decreased / grossly normal?
- Is RV contraction increased / decreased / grossly normal?
- Putting it together: What the ventricles can tell you in basic cardiac echo
THE QUESTIONS TO ASK
- Is left ventricle (LV) size big / small / grossly normal?
- Is LV contraction increased / decreased / grossly normal?
- Is right ventricle (RV) size big / small / grossly normal?
- Is RV contraction increased / decreased / grossly normal?
QUALITATIVE OR QUANTITATIVE?
– THE GOLDILOCKS APPROACH.
There are many ways to quantitatively measure these parameters, including the use of non-echo imaging modalities. Using ultrasound, there are many quantitative methods used, but in fact ‘eyeball assessment’ by an experienced echocardiographer is probably the most accurate. But even this is open to operator error!
In basic cardiac echo, stick to a qualitative assessment: the ‘Goldilocks approach’. This means that you won’t overcall pathology and you will also miss subtle disease such as diastolic heart failure and mild systolic failure.
The reason for adopting this approach rather than quantitative assessment is:
- You don’t have the time: this is a quick screening scan in the critically ill patient
- You don’t have the training: it takes years of full-time scanning to become proficient in formal TTE. Cardiac US is prone to trick the operator: there is plenty of artifact, and if the images obtained are non-standard (eg slicing through the LV at an angle), the operator can see pathology that simply isn’t there. This is why the echocardiographers teach that ‘you haven’t seen pathology unless you’ve seen it from two different windows.’
- You are combining this with scans of other areas eg lung, which will add information
- You are a clinician, and most of the important information will come from your clinical assessment.
IS LV SIZE BIG / SMALL / GROSSLY NORMAL?
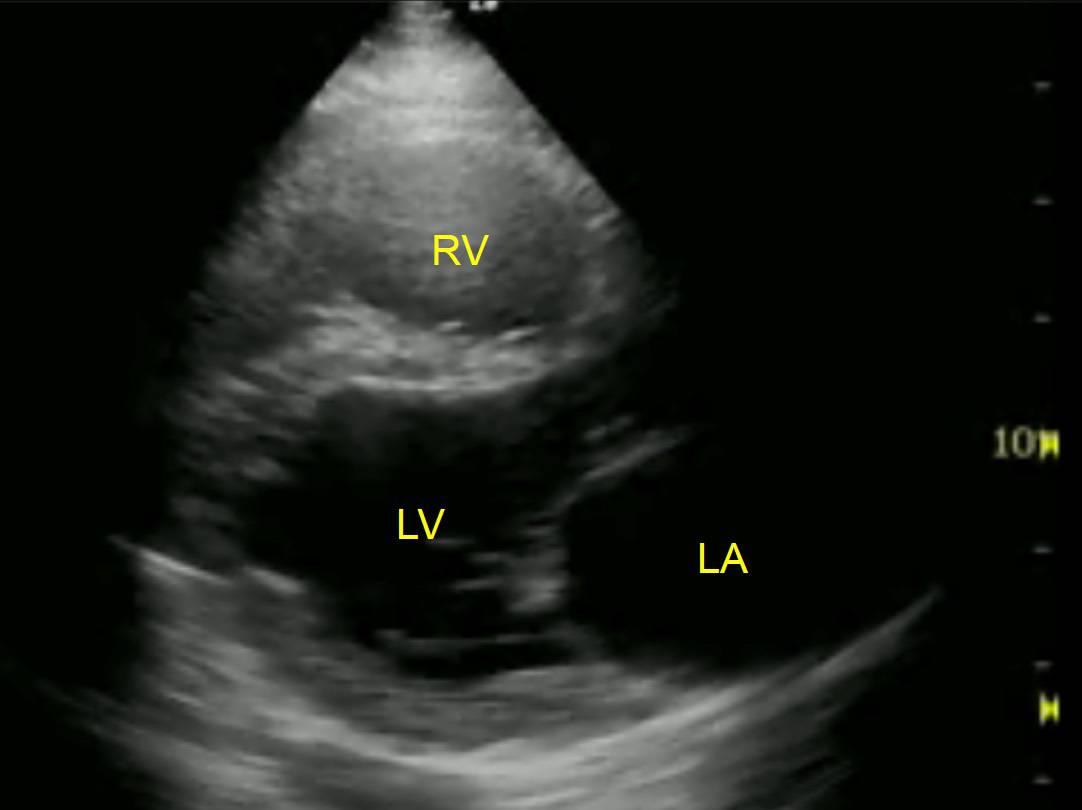
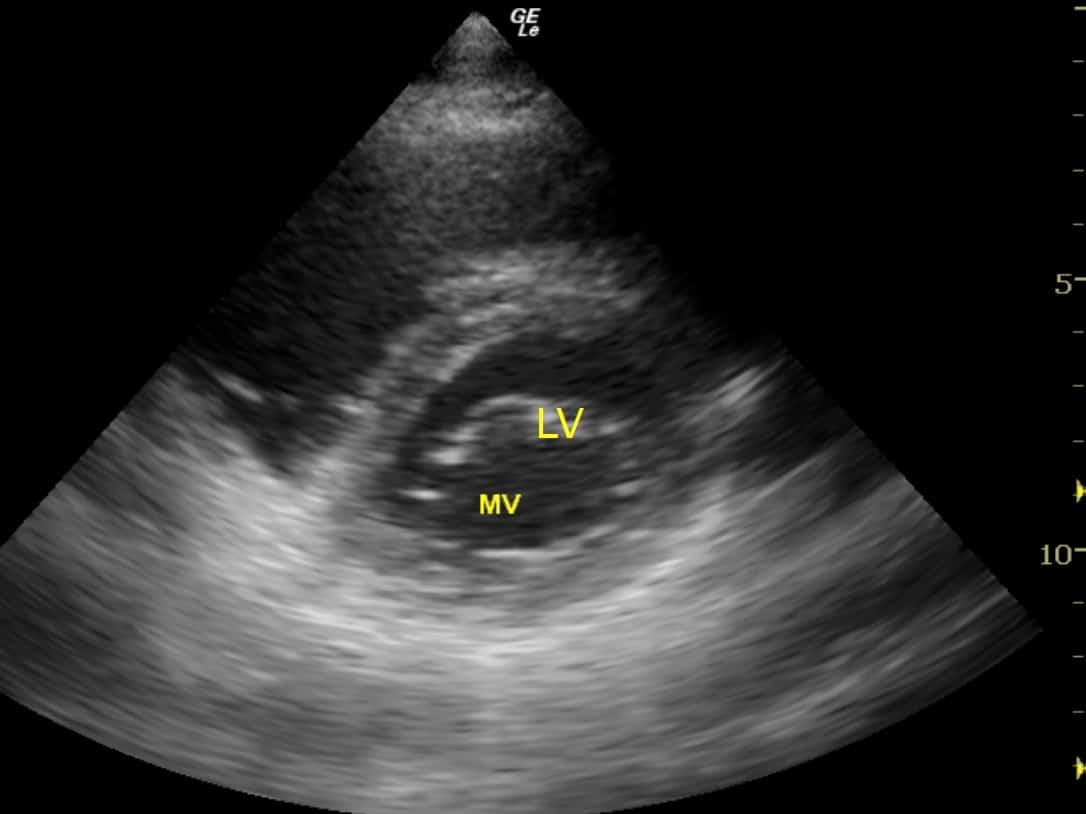
- Find a good view of the heart. The recommended window is the PLAX, but the PSAX isn’t bad (as long as it’s at the level of the mitral valve).
- Fan the probe back and forth until the LV appears largest.
- Freeze the image, then track back & forth until just before the LV contracts i.e. in diastole.
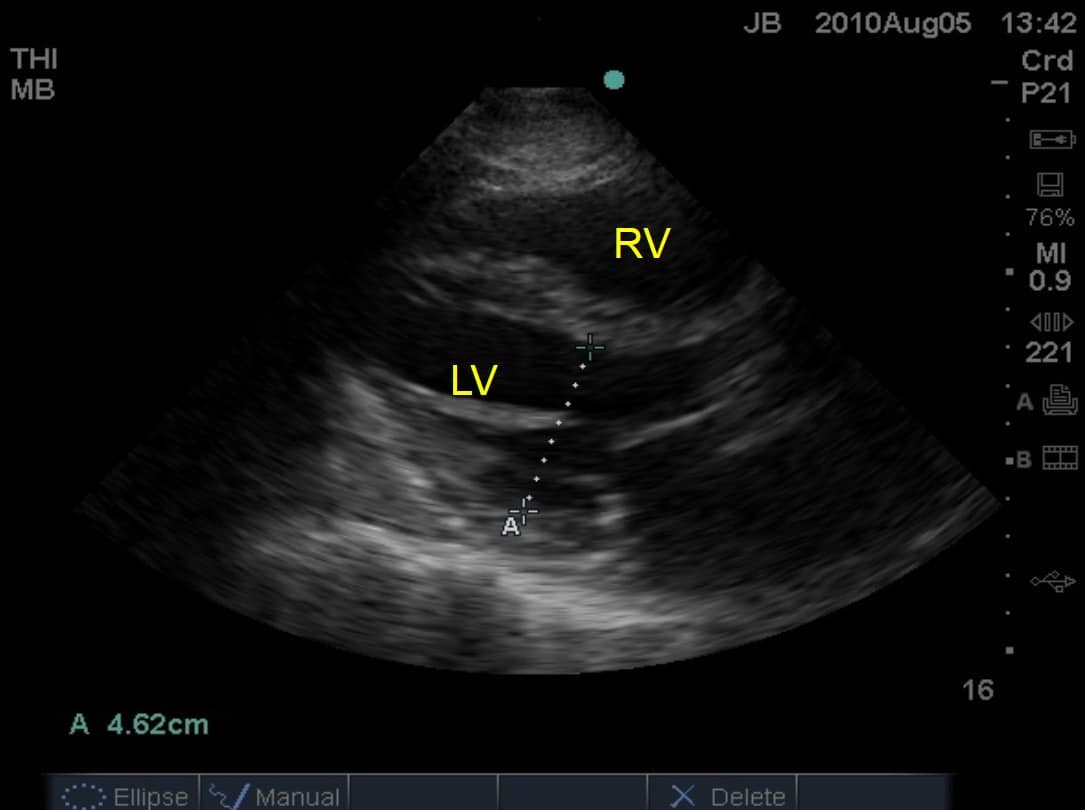
- Using the US calipers, measure the distance between the inner surface of the walls: this is the ‘LV internal diameter in diastole’ (LVIDd).
- Normal LV internal diameter (LVID) (in diastole) = 3.5-5.7cm (4-6cm roughly)
- But here’s the problem:
- These figures are averages only. They depend on factors such as sex (male usually bigger than female) and height (large people have large hearts).
- In a 2-minute scan, you haven’t much time! This means that many operators skip the measurement part and rely on eyeball assessment.
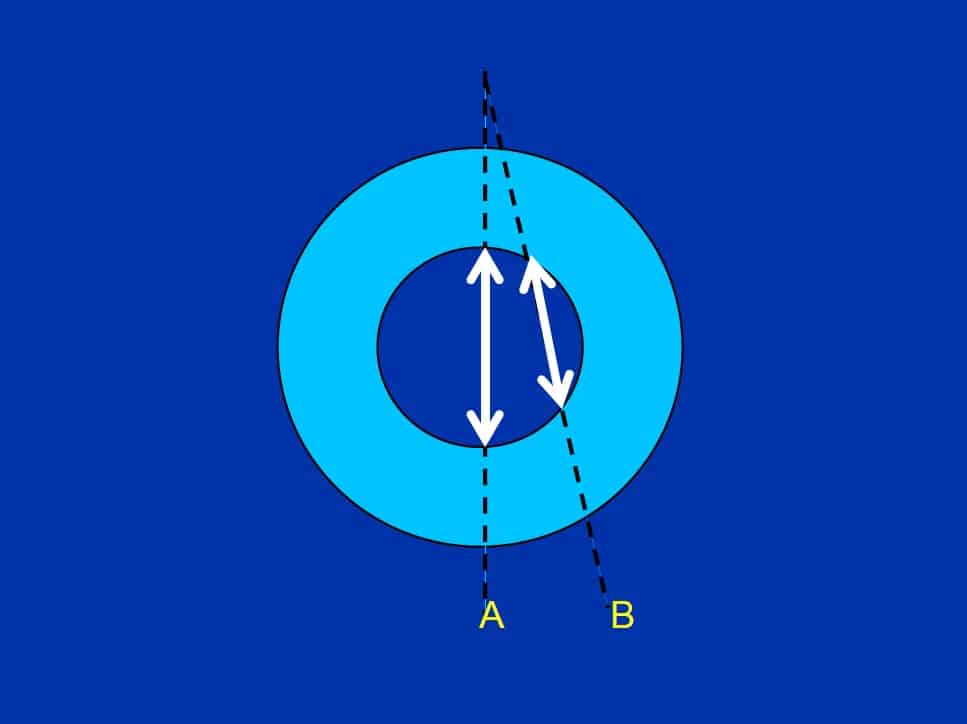
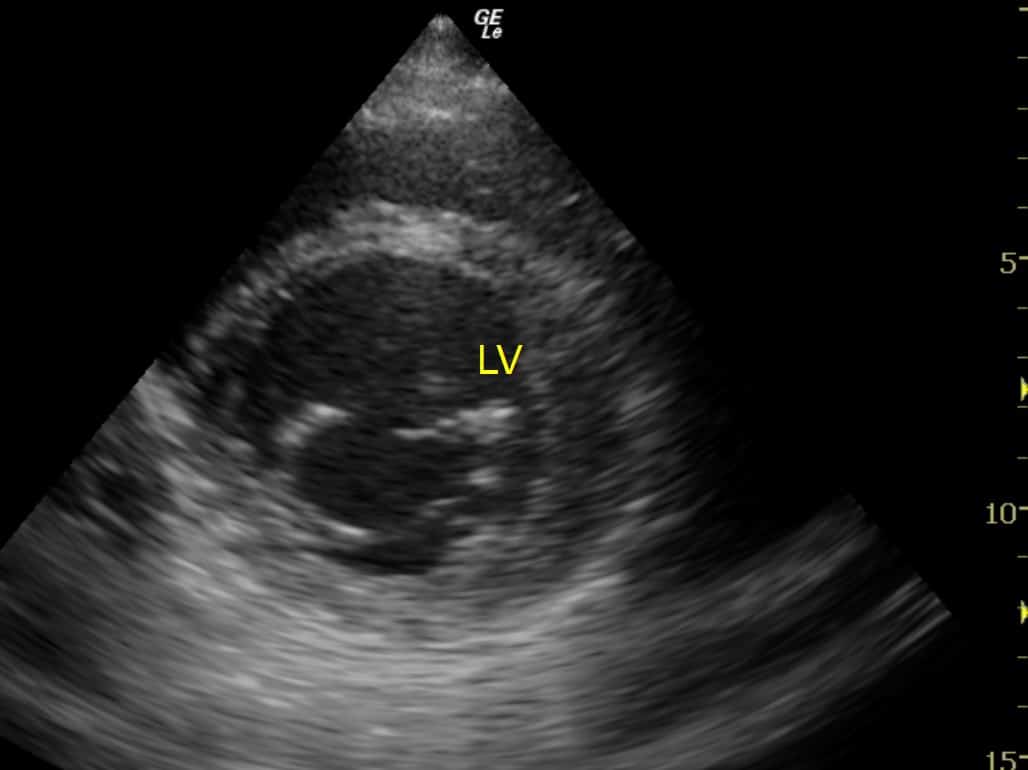
- It’s very easy to get this wrong: if your ‘line of sight’ is not through the true diameter, you’ll easily underestimate the LVID and will be puzzled why so many of your patients have small ventricles and thickened LV walls! (See figure below.)
-
The papillary muscles often get in the way, making the LV chamber size appear even smaller.
IS RV SIZE BIG / SMALL / GROSSLY NORMAL?
- A normal RV internal diameter in diastole (RVIDd) should be 2/3 or less of the LV.
- The exact figure is 0.9-2.6cm (1-3cm roughly) …once again, this depends on the size and sex of the patient.
- Most critical care clinicians will ‘eyeball’ the RV according to the following rule:
- Smaller than the LV = probably OK
- As large / larger than the LV = enlarged
- You can see that this formula will miss plenty of patients with subtly enlarged RV, but in the context of the critically ill patient this is not really a problem.
WHICH WINDOW?
- The best windows to assess RV size are the subcostal and A4C, because in the parasternal window, the RV lurks behind the sternum and is hard to see.
- But for the critical care physician, absolute RV size is often less important than RV pressure (see note below). The easiest way to assess this is often the PSAX window, to assess ‘bowing’ of the LV from a high pressure RV.
RV: INCREASED SIZE VERSUS INCREASED PRESSURE
WHAT’S THE DIFFERENCE?
- Of all 4 cardiac chambers, the RV is the one that dilates most rapidly with increased volumes (eg in fluid overload or LV failure).
- But a high pressure RV is a different beast: it implies an obstruction to flow between the 2 ventricles: cor pulmonale.
- The key difference on US is the behaviour of the IV septum (IVS). With high RV pressures, its usual ‘bulge’ towards the RV disappears or even reverses.
- In addition, the LV can appear ‘squashed’ by the higher pressure RV. On a PSAX view the LV loses its usual ‘O’ sign, replaced by a ‘D’.
ACUTE OR CHRONIC COR PULMONALE?
- An US finding of cor pulmonale is usually of great interest to the critical care physician. It can be acute (eg massive PE, tension PTX) or chronic (eg severe COPD, chronic lung fibrosis, primary pulmonary HT).
HOW TO TELL THEM APART?
- Acute cor pulmonale: RV free wall is still thin (< 0.6 cm in diastole)
- Chronic cor pulmonale: RV free wall has thickened to cope with the chronically high workload and is > 0.6 cm in diastole
-
In practice, measuring the RV free wall can be tricky. Clinical assessment (a good history and examination) can often pick them apart, but sometimes you’ll still be faced with a shocked, breathless patient who might have a massive PE, might have chronic cor pulmonale, or both. That’s one of the limitations of this test.
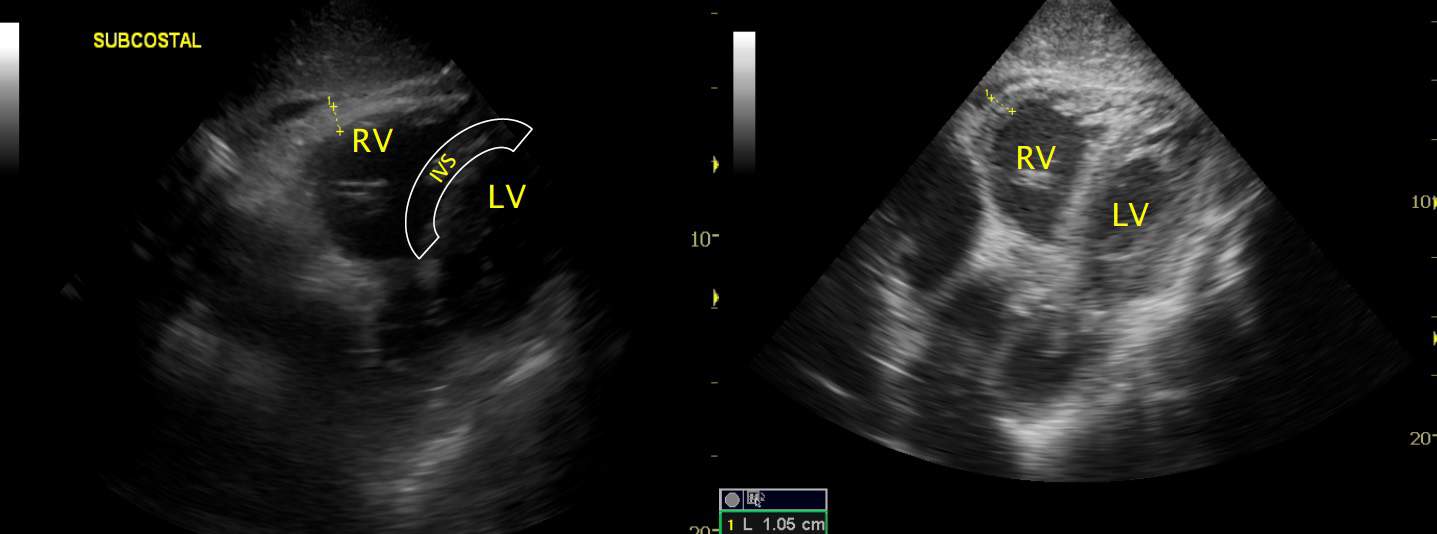
On the left, the RV pressure is lower than that in the LV, because their shared IV septum (IVS) still bulges toward the RV.
But on the right, the RV is higher pressure, the LV is ‘squashed’ and the IVS is flattened.
N.B. both cases are chronic: on the left, the RV free wall is 0.88cm. on the right, it’s 1.05cm.

On the left (normal heart), the RV pressure is lower than that in the LV, because their shared IV septum (IVS) bulges toward the RV. This is the ‘O’ sign, because the LV resembles an ‘O’ in cross section.
But on the right (cor pulmonale), the high-pressure RV ‘squashes’ the LV and flattens the IVS. This is the ‘D’ sign, because the LV resembles a ‘D’ in cross section.
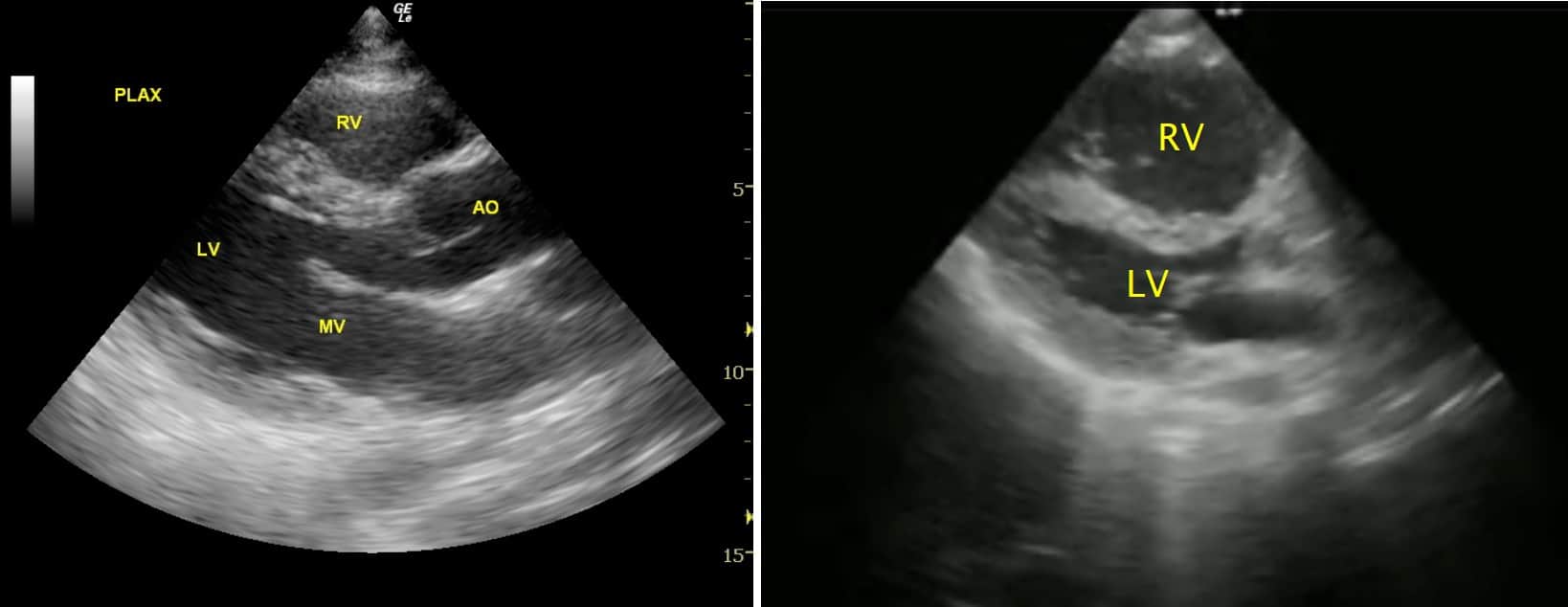
On the left (normal heart), the RV pressure is lower than that in the LV.
But on the right (cor pulmonale), the high-pressure RV ‘squashes’ the LV and flattens the IVS.
IS LV CONTRACTION INCREASED / DECREASED / GROSSLY NORMAL?
KEY POINTS:
- Quantitative measurement of LV systolic function takes more time than you have available in a resuscitation. With plenty of time and adequate training, one can apply calipers and compare the LVIDd, the LV cross-sectional area or even the LV volume in diastole and systole. From this you can derive the LV ejection fraction (LVEF) as a percentage. This takes several minutes.
- Measurement of LV diastolic function is even tougher. It requires tissue Doppler imaging, which is beyond most clinicians.
- Stick to a qualitative (Goldilocks) assessment of LV systolic function:
- Is it obviously increased?
- Is it obviously decreased?
- Is it grossly normal (and possibly subtly increased/decreased but probably not an issue in this critically ill patient?)
- What’s normal contraction? It’s hard to show on the page (it’s easier to see on cineloops or in real time scanning), but the normal LV contracts strongly and evenly towards its centre. The LV walls move simultaneously and thicken uniformly as they contract.
- What’s too much contraction? If the opposing LV walls touch as they contract, this is called ‘systolic kissing’. This is never normal. It occurs in:
- Hypovolaemia
- LV hypertrophy
- Hypertrophic obstructive cardiomyopathy (HOCM)
- What’s too little contraction? If the LV walls are barely moving, then that’s too little. (And yes, as usual this approach will miss milder cases.)
- What’s segmental hypokinesis? If a wall or a segment isn’t moving at all, the adjoining segments may drag it in a little as they contract, but it is moving only passively. It also won’t ‘thicken up’ in systole like the others. (This can be pretty hard to see at times.)
- What does an infarct look like? Although this is outside the bounds of CCUS, the classic US signs of an infarct include:
- Segmental akinesis/dyskinesis
- If chronic, thin-walled and bright (echogenic) because calcified
- Won’t this system mean that I miss a number of patients with even moderate heart failure? Yes. That’s a limitation of basic cardiac echo.
In this view, an eyeball assessment demonstrates the LV contracting, and its walls thickening, uniformly towards the centre of the ‘O’ without actually touching.
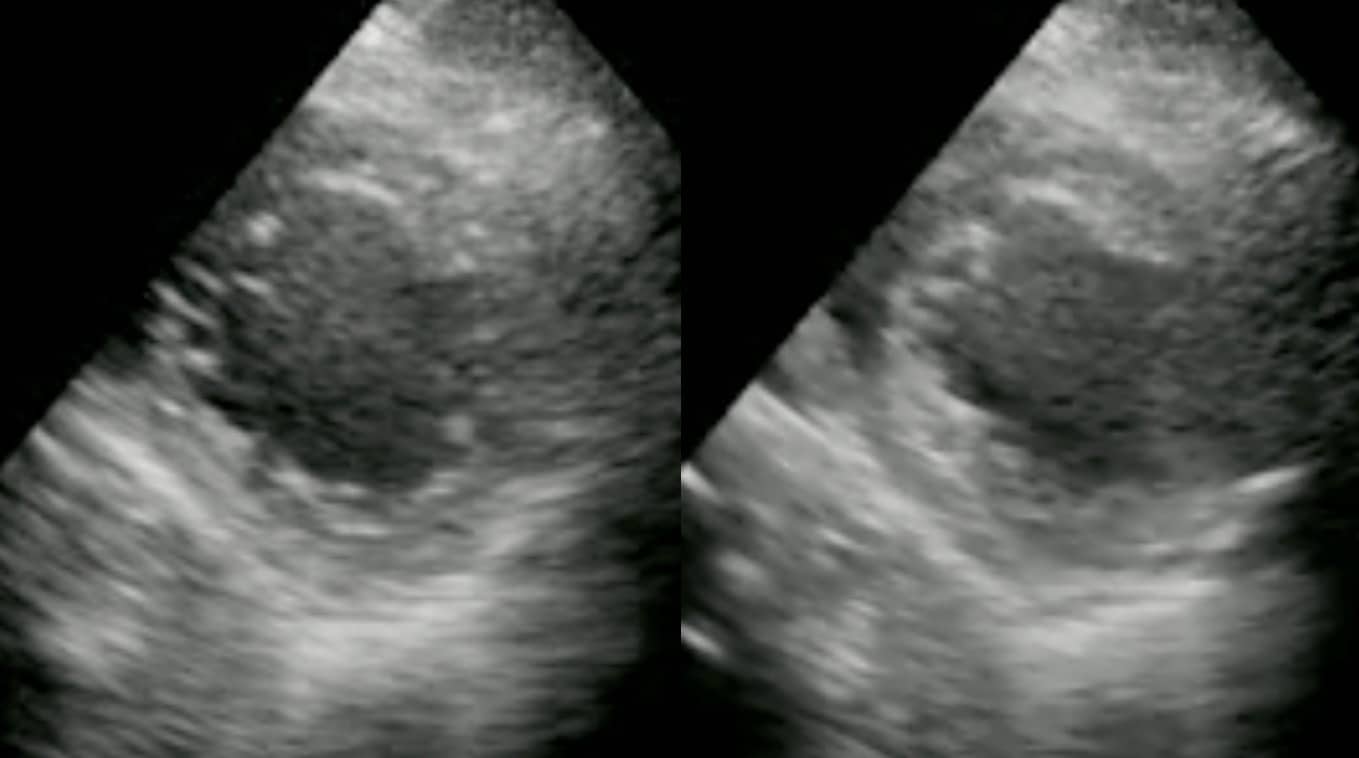
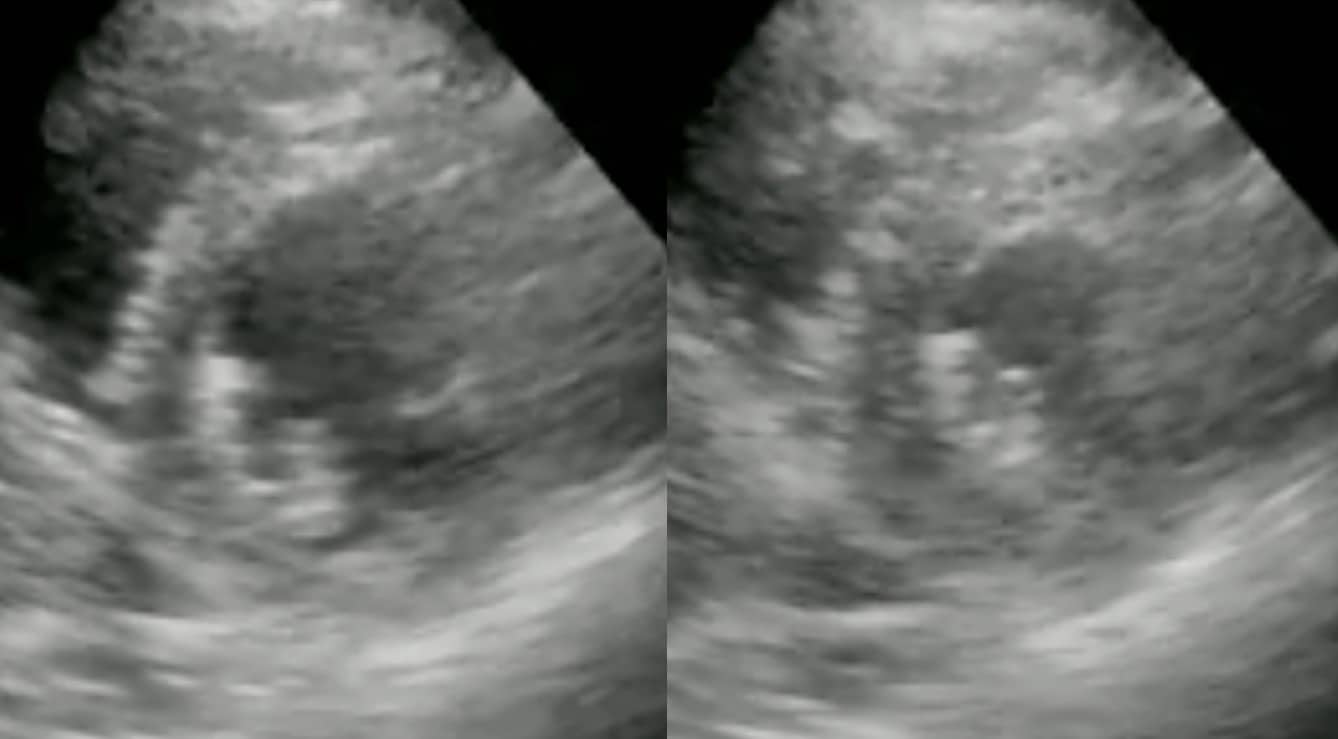
In this PSAX window, the LV is not formally measured but an eyeball assessment demonstrates that the diastolic dimensions (on the left) and systolic dimensions (on the right) are almost identical. Gross LV hypokinesis.
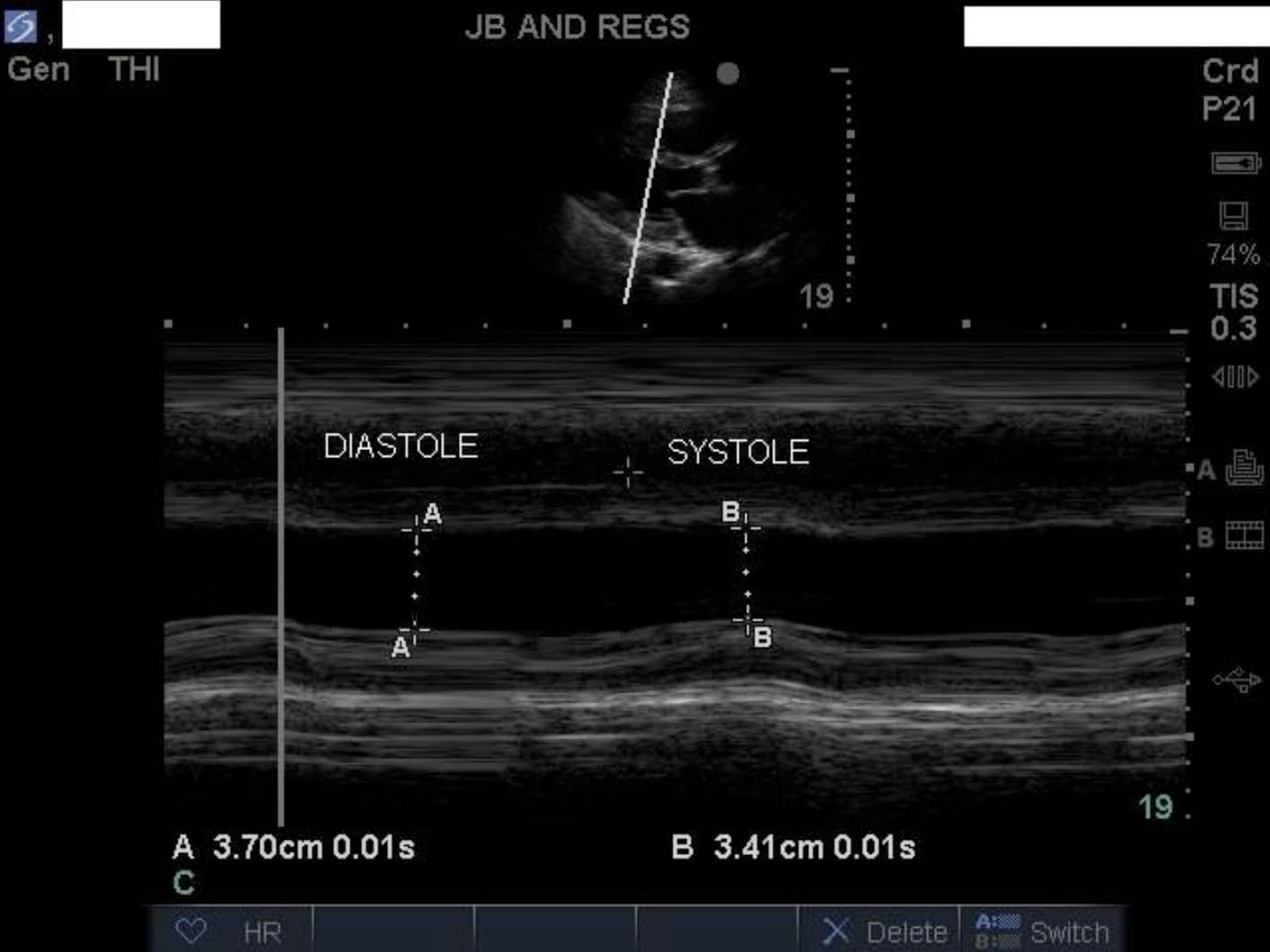
A = LV internal diameter in diastole (LVIDd) = 3.7cm
B = LV internal diameter in systole (LVIDs) = 3.4cm
In this view, the LV is contracting by only 10% = gross LV hypokinesis.
IS RV CONTRACTION INCREASED / DECREASED / GROSSLY NORMAL?
KEY POINTS:
Measurement of RV function is beyond the scope of basic cardiac echo. This is for the following
reasons:
- Measurement of RV function is even tougher than LV function. There are a number of reasons for this:
- The RV is harder to see (in the near field below the sternum on parasternal view)
- The RV is asymmetrical (unlike the cone shaped LV)
- The RV’s primary axis of contraction is its long axis. By comparison, the LV’s contraction is primarily concentric (but it also contracts along its long axis and also in a spiral). RV function is best assessed using motion of the tricuspid valve along the long axis of the heart. This is known as tricuspid annular peak systolic excursion (TAPSE).
- Most importantly: RV function is rarely a major issue in the critically ill patient.
PUTTING IT TOGETHER: WHAT THE VENTRICLES CAN TELL YOU IN BASIC CARDIAC ECHO
IS THIS HYPOVOLAEMIC SHOCK? LOOK FOR:
- Small, collapsing IVC (see IVC section)
- Small LV
- LV systolic kissing
IS THIS CARDIOGENIC SHOCK? LOOK FOR:
- Large IVC
- Large LV (only if chronic)
- LV may or may not be contracting ‘normally’ (basic echo will miss diastolic failure and mild systolic failure)
IS THIS SEPTIC SHOCK? THIS CAN BE TRICKY!
- IVC can be small (because of systemic vasodilation) or large (because of
hypocontractile heart)
- LV can be hyperkinetic (because of systemic vasodilation) or hypokinetic (because of hypocontractile heart)
IS THIS OBSTRUCTIVE SHOCK?
1. DOES THIS PATIENT HAVE A TENSION PTX?
- PTX seen on lung US
- IVC distended, non collapsing
- RV as large as the LV (or larger)
2. DOES THIS PATIENT HAVE A TAMPONADE? (SEE PERICARDIUM SECTION OF THIS MANUAL)
- IVC distended, non collapsing
- Pericardial fluid
- RV ‘squashed’ with diastolic collapse
3. DOES THIS PATIENT HAVE A PULMONARY EMBOLUS (PE)?
- Well, to be totally fair echo is not the most accurate of tests for a PE. Very occasionally it’ll pick up free thrombus in the pulmonary arteries, but most of the time it’s an indirect test, relying on signs such as:
- IVC distended, non collapsing
- RV as large as the LV (or larger)
- RV pressure > LV pressure (septum pushed towards LV)
- But it can’t rule out a small or even moderate PE.
- And it can be hard for any except the most experienced sonologists to differentiate acute cor pulmonale (eg massive PE) from chronic.
























